One-stage repair of hypospadias is currently fashionable and is undoubtedly attractive in concept but the methods that are presently available all have inherent limitations and drawbacks [22]. Children operated with single-stage tubed flap repairs such as the Broadbent and Mustarde techniques during the 1960s and 1970s, were found to have had a more than 90% complication rate at adult review [24].
The two-stage Bracka method offers a unique combination of versatility, reliability and refinement, and can be used for almost any hypospadias deformity, be it primary repair in a child or salvage surgery in an adult [22].
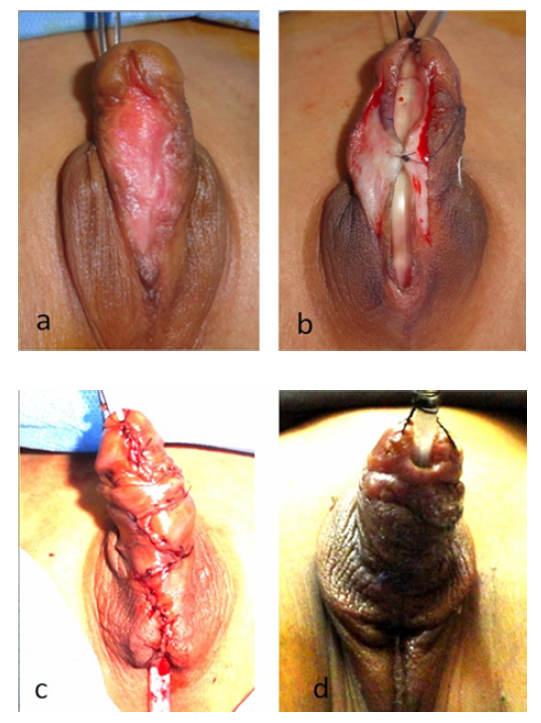
From the vast armamentarium of hypospadias repairs that are still in use, Dr. Aivar Bracka suggests a simple protocol of just three closely related procedures with which we can now repair almost all hypospadias. The tubularised incised plate (TIP) repair and the 'Snodgraft' modification of the TIP principle are simple and effective one-stage solutions when partial circumference urethroplasty is required. Conversely, the Bracka's two-stage graft repair remains an ideal and versatile solution when a full circumference urethroplasty is required. It is particularly appropriate for severe primary hypospadias associated with a poor plate and marked chordee and also to replace a scarred, hairy or balanitis xerotica obliterans diseased urethra in re-operative salvage hypospadias [19]. All single stage repairs have a limited range of application and therefore to deal with the full spectrum of hypospadias one has to master a variety of quite unrelated procedures and all the decision making that goes with them. By contrast, the two- stage method deals with everything from minor coronal hypospadias, through to the most severe proximal cases, even if circumcised or has already been the victim of multiple failed repairs [22]. The deep splitting of the glans in the 1.st stage making the tubularisation of the grafted area easy and free from tension, never the less the graft can be observed in the follow up period after the 1.st stage for any residual chordee or shallow glans, a problem can be corrected by revision of the 1.st stage by another smaller graft [22].
One-stage tubes have an inherent tendency to stricture, both at the junction with the native urethra and also at the meatus which therefore often finishes up as a puckered orifice rather than a normal slit. Attempts to prevent contraction of the meatus by coring out erectile tissue or turning in triangular glans flaps will further compromise the appearance of the glans. Two-stage Bracka's repair avoids this problem, producing a natural slit-shaped terminal meatus and an overall sophistication of result which is hard to match with the one-stage techniques [22].
The use of an intermediate or interposition layer between the neourethra and the skin layer has greatly improved the results following hypospadias surgery and reduced complications [8].
The Dartos fascia contains a pair of axial vessels which form an arterial network within the fascia which forms the basis of the axial tunica Dartos flap, In an attempt to decrease the occurrence of urethro-cutaneous fistula, Dartos fascia axial flap has been utilized as a vascularized layer over the tabularized urethra [5].
During the fifties of the last century a modification of a popular procedure (Thiersch Duplay) introduced by Byars. A potential problem with this Byars repair is that the urethral suture line faces the overlying skin closure and is therefore at significant risk of fistula formation [22].
Cesil A. B in 1946 described a method to repair proximal hypospadias with the use of single Z-plasty to close the penile shaft skin to balance between the short skin of the penoscrotal junction and the redundancy of the lateral one [25].
In more proximal hypospadias where there is sever curvature, the integumental volume deficiency will be very pronounced, and closing the defect by advancement of the edges would undoubtedly be associated with excessive tension, to solve this problem a Z-plasty could be carried out.
Furthermore the incorporation of Z-plasty to close the penile shaft skin certainly will overcome the problem of longitudinal facing between urethral suture line and the overlying skin closure and is therefore the risk of fistula formation will decrease which is the main indication of our choice for Z-plasty.
Bracka A. published his study on 600 hypospadias, including all types; result in a fistula rate (5.7%), in wich about (11-12%) in the 1.st three years. (7%) stricture rate. (3.7 %) underwent revision of the first stage of their repair. (5.5%) underwent further cosmetic adjustments after completion of their repairs [22].
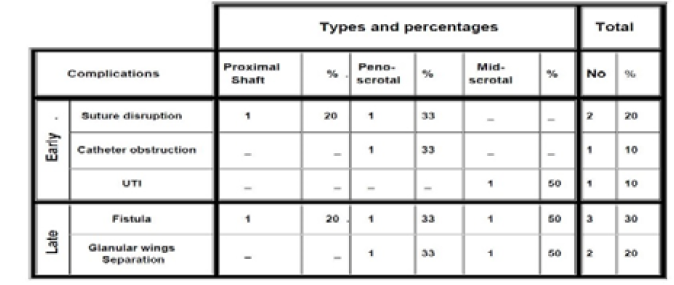
In our study which involve 5 cases (38%) proximal shaft , 5 cases (38%) peno- scrotal, whereas 3 cases( 23%) mid-scrotal type in the 1.st stage, and excluding one mid-scrotal , and two peno-scrotal cases from the 2.nd stage , with 2-6 months follow up period, there was 3 cases(30%) fistula all are in the earlier cases after second stage; this higher percentage perhaps due to the exclusive involvement of the proximal type, furthermore lower experience with this technique at the beginning of the study. This problem was canceled from the late 6 cases by increasing the depth of the glanular splitting in the first stage and change the site and direction of the corrugate drain from the proximal angle of the incision and longtudinal direction with the neourethral suture line to a site that pass between the two angles of the Z-plasty horizontaly.
Regarding other complications such as stricture, and meatal stenosis, in our study it is a 0%, this rate was due to the policy of our senior auther in delaying the stenting for 5-6 weeks and post-removal caliberation for another 2 months, but we need more follow up period to exclude possible future strictures.
There was 1 case (8% ) who require a revision for the 1.st stage due to mild residual chordee, which at 1.st was peno-scrotal with sever chordee. While in the follow up period of the 2.nd stage there was no residual chordee , also the technique of outer skin closure(Z-plastys) make a nice redistribution of the irregularly shaft and preputial skin , in addition to its favour of preventing facing between inner and outer suture lines. In Duckett's review of 18 patients undergoing to buccal mucosal grafting (16 tube) with 6-17 months follow up metal stenosis 28% which is 0% in our study. and fistula 6% in compare to 30% in our study .while in Woodard's review (Woodard's et al 1995) of 21 patients (proximal shaft: tubes and onlays) followed for 3-25 months whereas anastamosing stricture in 38%, and about 29% fistula rate which is approximately similar to our study[7], keeping in mind that we involve unselectively any proximal hypospadias whether operated or not.
Two cases (20%) in our study develop small distal glanular wings separation, and still they are satisfied and neglect its importance.
We agree with Aivar Bracka who state that, a further follow up is needed, as an ideal protocol should include an early evaluation within 3 months of surgery, followed by a review at 1 or 2 years, and again at 4 or 5 years [26].